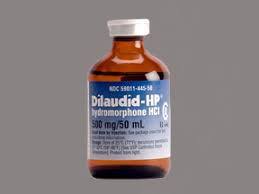
WARNING
Hydromorphone injection, like any medication, carries certain risks, especially when not used as prescribed. Some potential risks include:
- Addiction: Hydromorphone is an opioid pain medication, and like other opioids, it carries a risk of addiction or dependence, particularly with prolonged or high-dose use.
- Respiratory depression: High doses of hydromorphone can slow down breathing, leading to a dangerous condition called respiratory depression. This risk is higher in individuals with respiratory conditions or when combined with other central nervous system depressants like alcohol or benzodiazepines.
- Overdose: Taking too much hydromorphone can lead to overdose, which can be fatal. Symptoms of overdose include extreme drowsiness, slowed breathing, unconsciousness, and potentially coma or death.
- Tolerance and dependence: Over time, the body may develop a tolerance to hydromorphone, requiring higher doses to achieve the same pain relief. Dependence can also develop, leading to withdrawal symptoms if the medication is suddenly stopped.
- Constipation and other side effects: Common side effects of hydromorphone include constipation, nausea, vomiting, dizziness, and sedation. These side effects can be bothersome and may require additional medication to manage.
- Misuse and diversion: Hydromorphone is a potent opioid with a high potential for misuse and diversion. It’s important to use it only as prescribed and to store it securely to prevent unauthorized access.
Always follow your healthcare provider’s instructions carefully when taking hydromorphone injection, and be sure to discuss any concerns or questions with them.
Why is this medication prescribed?
Hydromorphone injection is typically prescribed for the management of severe pain that requires around-the-clock treatment and cannot be adequately controlled with other pain medications. It is commonly used in medical settings such as hospitals, clinics, or hospice care, especially for acute pain following surgery, trauma, or in cancer patients.
Hydromorphone belongs to the opioid class of pain medications, and it works by binding to opioid receptors in the brain and spinal cord, altering the perception of pain and producing feelings of relaxation and euphoria. Its rapid onset of action and potency make it particularly useful for severe pain situations where immediate relief is needed.
How should this medicine be used?
Hydromorphone injection should be used exactly as prescribed by a healthcare provider. Here are some general guidelines for its use:
- Dosage: The dosage of hydromorphone injection will vary depending on factors such as the severity of pain, the individual’s response to the medication, and any underlying medical conditions. It is important to follow the prescribed dosage carefully and not to exceed the recommended amount.
- Administration: Hydromorphone injection is typically administered by a healthcare professional in a hospital, clinic, or other medical setting. It may be given intravenously (IV), intramuscularly (IM), or subcutaneously (SC) depending on the specific situation and the patient’s needs.
- Frequency: The frequency of hydromorphone injections will also depend on the individual’s pain level and response to the medication. It is usually given on a scheduled basis for continuous pain relief, but additional doses may be administered as needed for breakthrough pain.
- Monitoring: While receiving hydromorphone injection, patients should be closely monitored for any signs of adverse effects or complications, such as respiratory depression, sedation, or changes in mental status. Vital signs, including blood pressure, heart rate, and respiratory rate, should be regularly checked.
- Disposal: Unused hydromorphone injection should be disposed of properly according to local regulations or guidelines to prevent misuse or accidental ingestion by others. It should not be shared with anyone else, even if they have similar symptoms.
- Caution with other medications: Hydromorphone injection can interact with other medications, especially other central nervous system depressants such as alcohol, benzodiazepines, or certain antidepressants. Patients should inform their healthcare provider of all medications they are taking to avoid potential interactions.
- Duration of use: Hydromorphone injection is typically used for short-term management of acute pain or for breakthrough pain in patients with chronic pain conditions. Prolonged or excessive use should be avoided due to the risk of tolerance, dependence, and other adverse effects.
It’s essential to follow all instructions provided by the healthcare provider and to communicate any concerns or questions about hydromorphone injection use.
Other uses for Ergoloid Mesylates
Other uses for Hydromorphone Injection may include:
- Management of pain in patients who are opioid-tolerant and require higher doses of opioid medication.
- Treatment of acute pain, such as postoperative pain, trauma-related pain, or pain due to medical conditions.
What special precautions should I follow?
Special precautions should be taken when using hydromorphone injection to minimize the risks associated with its use. Some important precautions include:
- Patient Evaluation: Before prescribing hydromorphone injection, healthcare providers should conduct a thorough evaluation of the patient’s medical history, including any history of substance abuse, respiratory conditions, or other factors that may increase the risk of complications.
- Dosage Adjustment: The dosage of hydromorphone injection should be carefully adjusted based on the patient’s individual response to the medication, pain level, and other factors. Lower doses are typically recommended for elderly patients, patients with renal or hepatic impairment, and those who are opioid-naive.
- Respiratory Monitoring: Patients receiving hydromorphone injection should be closely monitored for signs of respiratory depression, especially during initiation of therapy and dose adjustments. Vital signs, including respiratory rate and oxygen saturation, should be regularly assessed.
- Caution with Central Nervous System Depressants: Hydromorphone injection can potentiate the sedative effects of other central nervous system depressants, such as alcohol, benzodiazepines, and certain antidepressants. Concurrent use should be avoided or closely monitored.
- Constipation Management: Opioid-induced constipation is a common side effect of hydromorphone injection and should be proactively managed with laxatives or other bowel regimen to prevent complications.
- Pregnancy and Lactation: Hydromorphone injection should be used with caution in pregnant or breastfeeding women, as it may cause adverse effects in the fetus or newborn. The potential benefits and risks should be carefully weighed, and alternative treatments may be considered.
- Risk of Dependence and Withdrawal: Prolonged use of hydromorphone injection can lead to physical dependence, and abrupt discontinuation may precipitate withdrawal symptoms. Tapering the dosage gradually under medical supervision is recommended when discontinuing treatment.
Patients should always follow their healthcare provider’s instructions and communicate any concerns or adverse effects while using hydromorphone injection.
What special dietary instructions should I follow?
There are no specific dietary restrictions associated with hydromorphone injection. However, maintaining a healthy and balanced diet can support overall health and well-being, which may indirectly impact your response to pain management.
What should I do if I forget a dose?
If you forget a dose of hydromorphone injection, take it as soon as you remember. However, if it is almost time for your next scheduled dose, skip the missed dose and continue with your regular dosing schedule. Do not double the dose to catch up. If you are unsure about what to do, contact your healthcare provider for guidance.
What side effects can this medication cause?
Hydromorphone injection, like other opioid medications, can cause a range of side effects. Common side effects may include:
- Nausea and vomiting: These gastrointestinal symptoms are relatively common, especially when starting treatment or with higher doses.
- Constipation: Opioids can slow down bowel movements, leading to constipation. It’s important to maintain adequate hydration, dietary fiber intake, and, if necessary, use laxatives as directed by your healthcare provider to manage this side effect.
- Dizziness and drowsiness: Hydromorphone can cause central nervous system depression, resulting in feelings of dizziness or excessive sleepiness.
- Sedation: Some individuals may experience sedation or a feeling of mental clouding while taking hydromorphone.
- Respiratory depression: In high doses or in susceptible individuals, hydromorphone can suppress breathing, leading to respiratory depression. This is a potentially serious side effect that requires immediate medical attention.
- Itching or rash: Some people may experience itching or skin rash as a side effect of hydromorphone.
- Headache: Headaches are a relatively common side effect of opioid medications.
- Sweating: Excessive sweating, especially at night, can occur with hydromorphone use.
- Dry mouth: Opioids can cause dry mouth, which may contribute to dental issues if not managed properly.
- Urinary retention: Difficulty or inability to urinate can occur as a result of hydromorphone use.
Less common but more serious side effects of hydromorphone injection may include allergic reactions, serotonin syndrome (if used concomitantly with certain other medications), adrenal insufficiency, and tolerance, dependence, or addiction with prolonged use.
It’s important to report any concerning or persistent side effects to your healthcare provider. Additionally, seek immediate medical attention if you experience signs of respiratory depression, such as slow or shallow breathing, or any other severe or life-threatening symptoms.
What should I know about storage and disposal of this medication?
When it comes to storage and disposal of Hydromorphone Injection, here’s what you should know:
Storage:
- Store hydromorphone injection at room temperature, away from light and moisture.
- Keep it out of reach of children and pets, as accidental ingestion can be fatal.
- Do not share your medication with others, even if they have similar symptoms.
- Follow any specific storage instructions provided by your pharmacist.
Disposal:
- Dispose of unused or expired hydromorphone injection properly according to local regulations or guidelines.
- Do not flush medications down the toilet unless instructed to do so.
- Many pharmacies and healthcare facilities have medication take-back programs or can provide guidance on safe disposal methods.
In case of emergency/overdose
- If you or someone else may have overdosed on hydromorphone, call emergency services (such as 911 in the United States) immediately.
- While waiting for help to arrive, try to keep the person awake and breathing.
- If possible, provide emergency responders with information about the medication taken, including the dosage and when it was taken.
What other information should I know?
- Avoid drinking alcohol or taking other central nervous system depressants while using hydromorphone, as it can increase the risk of respiratory depression and other adverse effects.
- Inform your healthcare provider about all medications you are taking, including prescription, over-the-counter, and herbal supplements, to avoid potential interactions.
- Do not drive or operate heavy machinery until you know how hydromorphone affects you, as it can cause dizziness, drowsiness, and impaired judgment.
- Do not suddenly stop taking hydromorphone without consulting your healthcare provider, as it can cause withdrawal symptoms. Your doctor can provide guidance on tapering the medication safely if needed.
- Keep all appointments with your healthcare provider for monitoring and evaluation of your response to hydromorphone treatment.
Following these guidelines can help ensure the safe and effective use of hydromorphone injection. If you have any questions or concerns, don’t hesitate to discuss them with your healthcare provider.